Introduction
Teenage acne is often assumed to be a simple or temporary part of growing up, yet in practice, it can present in different ways and persist for varying lengths of time. For some, it remains mild and manageable, while for others it becomes more widespread, inflamed, or resistant to standard skincare. This variation can make it difficult to understand what is normal, what requires treatment, and which options are appropriate at different stages.
There is also a significant amount of conflicting information surrounding acne, particularly online. Advice on skincare routines, diet, and treatments is often inconsistent and not always aligned with clinical guidance. This can lead to unnecessary trial and error, delayed treatment, or concern about whether the right steps are being taken. A clearer understanding of how acne develops and how it is assessed can help reduce this uncertainty.
This guide provides a structured overview of teenage acne in the UK, including how it forms, the different types and triggers, and the range of treatment pathways available. It also outlines what to expect from treatment over time, when to seek professional advice, and how to reduce the risk of longer-term skin changes such as scarring.
Understanding how teenage acne develops is a useful starting point for making sense of treatment options and expectations.
LDM® Triple
LDM® Triple is a non-invasive ultrasound-based treatment used in aesthetic and dermatology clinics to support skin health, tissue regulation, and the Treatment of Acne-Prone or inflamed skin. This guide is for anyone trying to understand what it is, how it works, and whether it may be relevant to their skin concern.
- What LDM® Triple is, and how it differs from standard cosmetic ultrasound
- Which skin concerns it is commonly used for, including Acne and early ageing-related concerns
- What to consider around suitability, comfort, risks, pricing and provider choice
Visit Website
What Is Teenage Acne And Why Does It Happen?
Teenage acne is a common skin condition that develops during puberty, when hormonal changes increase oil production and make pores more likely to become blocked.
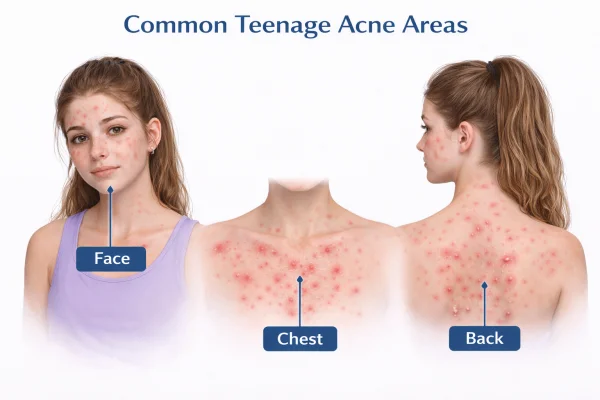
How acne develops in teenage skin
-
Acne begins in the hair follicles, which are small openings in the skin connected to oil-producing glands.
-
During puberty, these glands produce more sebum (oil) than the skin needs.
-
Excess oil mixes with dead skin cells, forming a plug that blocks the pore.
-
This environment allows naturally occurring bacteria to multiply, leading to inflammation and visible spots.
-
Depending on the severity of the blockage, this can result in blackheads, whiteheads, or inflamed lesions.
The role of hormones during puberty
-
Hormonal changes, particularly increased androgens such as testosterone, stimulate the sebaceous glands.
-
This affects both males and females, even though hormone patterns differ.
-
Acne often begins between the ages of 11 and 14, but timing varies.
-
Breakouts may fluctuate as hormone levels change, which is why acne can appear unpredictable.
Difference between normal breakouts and acne
-
Occasional spots can happen at any age and usually resolve quickly.
-
Acne is typically persistent, with repeated breakouts in the same areas.
-
Signs of acne include:
-
Acne may affect the face, chest, back, or shoulders, often in patterns linked to oil production.
Teenage acne develops as a natural response to hormonal changes, rather than anything related to hygiene or lifestyle alone. Understanding this helps set realistic expectations and supports a more structured approach to treatment.
Types Of Teenage Acne And How To Recognise Them
Understanding the different types of teenage acne helps clarify why some breakouts respond quickly to treatment, while others require a more structured approach.
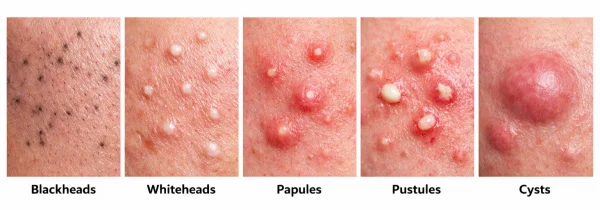
Comedonal acne (blackheads and whiteheads)
-
This form of acne is non-inflammatory, meaning there is no redness or swelling.
-
It develops when pores become blocked with oil and dead skin cells.
-
Blackheads remain open at the surface and appear dark due to oxidation, not dirt.
-
Whiteheads are closed and appear as small, pale bumps under the skin.
-
Typically found on the forehead, nose, and chin.
-
Semantic relevance: blackheads vs whiteheads, comedonal acne in teenagers
-
Common concern addressed: “Why do I have bumps but no inflamed spots?”
Inflammatory acne (papules and pustules)
-
Occurs when blocked pores become inflamed due to bacterial activity.
-
Papules are small, red, raised spots without visible pus.
-
Pustules contain pus and often appear with a white or yellow centre.
-
These lesions may feel tender and can persist longer than comedonal acne.
-
More common across the cheeks, jawline, chest, and back.
-
Semantic relevance: inflamed acne in teenagers, papules and pustules meaning
-
Common concern addressed: “Why do my spots become red and sore?”
Nodular and cystic acne
-
This is a more severe form of acne, involving deeper inflammation within the skin.
-
Nodules are firm, painful lumps beneath the surface.
-
Cysts are larger, pus-filled lesions that may remain for weeks.
-
Higher risk of scarring and long-term skin changes if not managed early.
-
Often requires medical assessment and prescription treatment.
-
Semantic relevance: cystic acne in teenagers UK, severe acne signs
-
Common concern addressed: “When should I seek professional advice?”
Recognising the type of acne present is an important step in choosing appropriate treatment and avoiding unnecessary trial and error.
Common Triggers And Worsening Factors In Teenagers
Teenage acne is primarily driven by internal changes, but certain external factors can influence its severity or persistence.
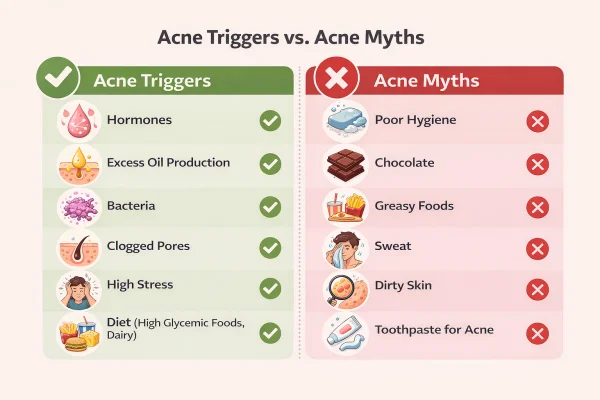
Hormones and natural oil production
-
During puberty, increased hormone levels stimulate the sebaceous glands to produce more oil.
-
This excess oil makes pores more likely to become blocked and inflamed.
-
Hormonal fluctuations can lead to cycles of breakouts, even when skincare is consistent.
-
This process is largely biological and not directly controllable, which is important to recognise early.
-
Semantic relevance: teenage acne hormones explained, puberty acne causes
-
Common concern addressed: “Is there anything I can do to stop hormonal acne?”
Skincare and cosmetic products
-
Some products can block pores, particularly those labelled as oil-based or comedogenic.
-
Over-cleansing or using harsh scrubs can disrupt the skin barrier, increasing irritation.
-
Using multiple active ingredients at once may worsen redness and sensitivity.
-
Choosing non-comedogenic, fragrance-free products can help reduce unnecessary irritation.
-
Semantic relevance: skincare mistakes, acne, teenagers, products that cause acne
-
Common concern addressed: “Am I making my acne worse with the products I use?”
Lifestyle influences (diet, stress, and environment)
-
There is limited evidence linking specific foods directly to acne, although high glycaemic diets may play a role in some individuals.
-
Stress can influence hormonal activity, which may contribute to flare-ups.
-
Sweat, friction from clothing, and sports equipment can trap oil and bacteria against the skin, particularly on the back and shoulders.
-
Environmental factors, such as humidity or occlusive clothing, can also contribute.
-
Semantic relevance: does diet affect acne UK, sports acne, and teenagers
-
Common concern addressed: “Do I need to change my diet or lifestyle?”
While teenage acne cannot always be prevented, understanding common triggers can help reduce unnecessary aggravation and support more consistent skin management.
How Teenage Acne Is Assessed And When To Seek Help
Teenage acne is usually straightforward to assess, but understanding when to seek help can make a meaningful difference to both outcomes and long-term skin health.
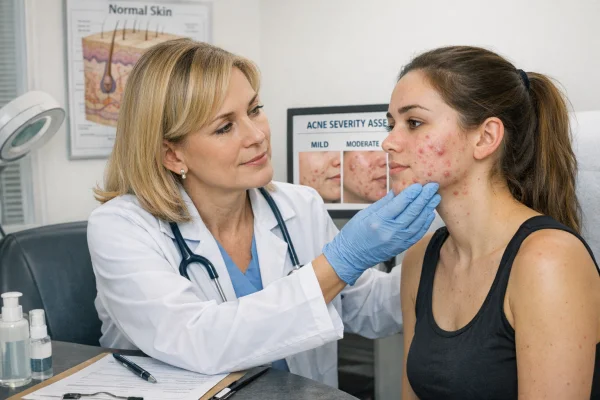
How GPs and clinicians assess acne
-
Acne is diagnosed through a visual examination of the skin, rather than tests or scans.
-
Clinicians look at:
-
The type of lesions present, such as blackheads, inflamed spots, or deeper nodules
-
The distribution of acne, for example, the face, chest, or back
-
The severity and persistence over time
-
Acne is typically classified as mild, moderate, or severe, which helps guide treatment decisions.
-
This assessment also considers whether there are early signs of scarring or pigmentation changes.
-
Semantic relevance: acne diagnosis UK, how doctors assess acne
-
Common concern addressed: “Will I need tests or investigations?”
When acne needs medical treatment
-
Many cases of mild acne can be managed with pharmacy advice and consistent skincare.
-
Medical treatment is usually recommended when:
-
Acne is persistent or worsening despite over-the-counter options
-
There are painful or deep lesions, such as nodules or cysts
-
Acne is starting to leave marks or scars
-
Breakouts are affecting confidence or wellbeing
-
Early intervention can reduce the risk of long-term skin changes.
-
Semantic relevance: when to see a GP for acne in the UK
-
Common concern addressed: “Is my acne serious enough to see a doctor?”
Referral to dermatology services
-
Referral may be considered if:
-
Acne does not respond to standard treatments
-
There is moderate to severe acne, particularly with scarring risk
-
There is diagnostic uncertainty or an underlying medical factor
-
In the UK, this may involve:
-
Specialist care allows access to treatments such as oral isotretinoin, which require careful supervision.
-
Guidance emphasises that treatment should be reviewed over structured periods, often around 12 weeks, to assess response and adjust if needed.
-
Semantic relevance: dermatologist referral acne UK
-
Common concern addressed: “What happens if standard treatments do not work?”
Assessment of teenage acne is based on visible signs and severity, with referral considered when acne is persistent, severe, or affecting wellbeing.
Teenage Acne Treatment Options In The UK
Teenage acne treatment options in the UK vary depending on severity, with most approaches following a structured pathway that balances effectiveness with safety.
Over-the-counter treatments and skincare
-
Often, the first step is for mild acne or early breakouts.
-
Common options include:
-
Benzoyl peroxide, which reduces bacteria and inflammation
-
Gentle, non-comedogenic cleansers and moisturisers
-
Products should be used consistently, usually once or twice daily, depending on tolerance.
-
Harsh or overly complex routines can increase irritation and reduce adherence.
-
Semantic relevance: best acne products for teenagers in the UK, over-the-counter acne treatment in the UK
-
Common concern addressed: “Where should I start with treatment?”
Prescription treatments from a GP
-
Recommended when acne is persistent or moderate in severity.
-
Options may include:
-
Topical retinoids, which help prevent blocked pores
-
Combination treatments with benzoyl peroxide and antibiotics
-
Treatment is usually prescribed as a 12-week course, with review at the end of this period.
-
Visible improvement often takes 6 to 8 weeks, so early patience is important.
-
Semantic relevance: prescription acne treatment UK teens, GP acne treatment UK
-
Common concern addressed: “How long before treatment starts working?”
Treatments for moderate to severe acne
-
For more widespread or persistent acne, oral treatments may be considered.
-
These can include:
-
Oral antibiotics, used alongside topical treatments
-
Hormonal treatments in selected cases
-
Oral isotretinoin, reserved for severe or treatment-resistant acne
-
These options require clinical supervision, with careful discussion of risks and suitability.
-
Treatment choice depends on factors such as age, severity, and previous response.
-
Semantic relevance: severe acne treatment for teenagers in the UK, isotretinoin UK acne
-
Common concern addressed: “Are stronger treatments safe and when are they needed?”
Professional clinic treatments
-
It may be used alongside medical treatment or when additional support is needed.
-
Options available in UK clinics include:
-
Chemical peels, which help exfoliate and reduce blocked pores
-
Light-based therapies, targeting inflammation and bacteria
-
Ultrasound-based treatments such as LDM Triple, which support skin repair and barrier function
-
These treatments are typically adjunctive, meaning they support rather than replace medical care.
-
Suitability depends on the type of acne, skin sensitivity, and the overall treatment plan.
-
Semantic relevance: acne clinic treatments UK, LDM Triple acne treatment
-
Common concern addressed: “Do clinic treatments offer real benefits or are they optional?”
Treatment for teenage acne is most effective when matched to severity and followed consistently over time, rather than changed frequently.
What Results To Expect And How Long Treatment Takes
Understanding how long acne treatment takes helps set realistic expectations and reduces the risk of stopping too early.

Typical acne treatment timelines
-
Most treatments take 6 to 8 weeks for noticeable improvement to begin.
-
A full assessment is usually made around 12 weeks, which is why many treatments are prescribed in structured courses.
-
Early stages may show subtle changes, such as fewer new spots rather than immediate clearing.
-
More significant improvement often develops gradually over time.
-
Semantic relevance: how long acne treatment takes in the UK, acne treatment timeline
-
Common concern addressed: “Why is my skin not improving yet?”
Managing initial flare-ups or irritation
-
Some treatments, particularly retinoids, can cause temporary irritation or dryness.
-
A short-term increase in breakouts may occur as the skin adjusts.
-
This does not necessarily mean the treatment is unsuitable, but it may need:
-
Persistent or severe irritation should be reviewed with a clinician.
-
Semantic relevance: acne treatment purge UK, retinoid irritation acne
-
Common concern addressed: “Is my treatment making my acne worse?”
Importance of consistency and follow-up
-
Consistent use is essential, as irregular application can reduce effectiveness.
-
Stopping treatment early may lead to recurrence of breakouts.
-
Follow-up allows:
-
Adjustment of treatment strength or type
-
Monitoring for side effects
-
Consideration of alternative options if needed
-
Treatment plans are often stepped or combined, depending on response.
-
Semantic relevance: acne treatment consistency importance, acne follow-up UK
-
Common concern addressed: “Can I stop treatment once my skin improves?”
Acne treatment works gradually, with improvement building over weeks rather than days, making consistency and review an important part of the process.
Preventing Acne Scars And Long-term Skin Damage
Preventing acne scars is a key part of managing teenage acne, as early and consistent treatment can reduce the likelihood of lasting skin changes.
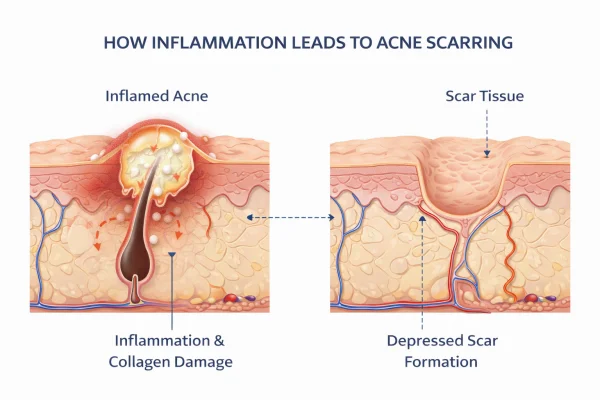
Why acne scars develop
-
Scarring occurs when inflammation damages deeper layers of the skin.
-
More severe acne, such as nodules and cysts, carries a higher risk.
-
Delayed or ineffective treatment can allow inflammation to persist, increasing this risk.
-
Repeated breakouts in the same area may also contribute to long-term changes.
-
Semantic relevance: how acne scars form in teenagers, acne scarring causes
-
Common concern addressed: “Will my acne leave permanent marks?”
Practical steps to reduce scarring risk
-
Avoid picking or squeezing spots, as this increases inflammation and skin trauma.
-
Start appropriate treatment early to reduce the duration of active acne.
-
Use non-comedogenic skincare to support the skin barrier.
-
Apply daily sun protection, as UV exposure can worsen post-acne pigmentation.
-
Follow treatment plans consistently to reduce repeated flare-ups.
-
Semantic relevance: prevent acne scars in UK teens, acne scar prevention tips
-
Common concern addressed: “What can I do now to protect my skin?”
When to treat acne scars
-
Some marks, such as post-inflammatory pigmentation, may fade over time.
-
True scarring, including indentations or raised areas, may require treatment.
-
Options in clinical settings can include:
-
Treatment is usually considered once acne is stable and under control.
-
Semantic relevance: acne scar treatment UK overview, treating acne scars options
-
Common concern addressed: “Can scars be treated later if they develop?”
Reducing inflammation early and avoiding unnecessary skin trauma are the most effective ways to lower the risk of acne scarring.









